Will health reforms deliver better health care?
With huge restructuring now underway, local HB health providers respond.
“I want to have the same chance as my Pākeha friends to watch my 11-year-old boy grow up and have kids – it’s not a big ask – yet because I am Māori, I am statistically likely to die seven and half years earlier.”
For Nathan Harrington CEO of Te Kupenga Hauora – Ahuriri, a kaupapa Māori-driven health and social service provider, this is the depressing and graphic reality behind the oft-quoted example of health inequity in New Zealand.
“The figures don’t lie,” he says. “The current health system is not working. There are poorer outcomes for Māori and Pacific and multiple reviews have shown us that Māori just don’t have the same access to health delivery and specialist services as non-Māori.”
In a newly-reformed health system, Harrington wants reassurance that if he gets sick and needs to be referred to a specialist like an oncologist, he will be at the same rate as his non-Māori friends. “That if I turn up at a GP, I will get the medicine I need at the same rate as my non-Māori friends – and won’t be given a lecture on lifestyle.”
Harrington (Rongomaiwahine, Ngāi Tamanuhiri and Rongowhakaata) has worked for numerous Māori health providers, been employed in the Public Service and was involved in the early stages of the establishment of the Whānau Ora Commissioning Agency. He is one of numerous people I have spoken to as I have tried to get a sense what Labour’s Pae Ora, (Healthy Futures) bill might mean for Hawke’s Bay when it becomes law on 1 July.
Structural change
As BayBuzz readers open their new July/August magazine, District Health Boards (DHBs) with their elected members – those names we’re meant to tick on Local Body Election Voting Papers but often don’t because we don’t know who they are – will be gone!
Ironically it was a Labour Government in 2000 who set up DHBs replacing a National Government’s centralised Health Funding Agency and four Regional Health Authorities.
Now the dissolution of the 20 DHBs around New Zealand is the first step in a massive re-configuring and re-nationalising of our health system with a whopping $11.1 billion tagged in May 2022’s Budget for the health reforms over the next four years.
The reforms have come out of the 2018 Health and Disability review and are underpinned by two key findings: 1) that we need to tackle the persistent inequity in health outcomes for Māori and Pacific peoples, and 2) that the DHB system has delivered unequal access to health services depending where you live in New Zealand.
“We need this shake up,” says Tukituki Labour MP Anna Lorck. “A new system will deliver better outcomes for all of us.”
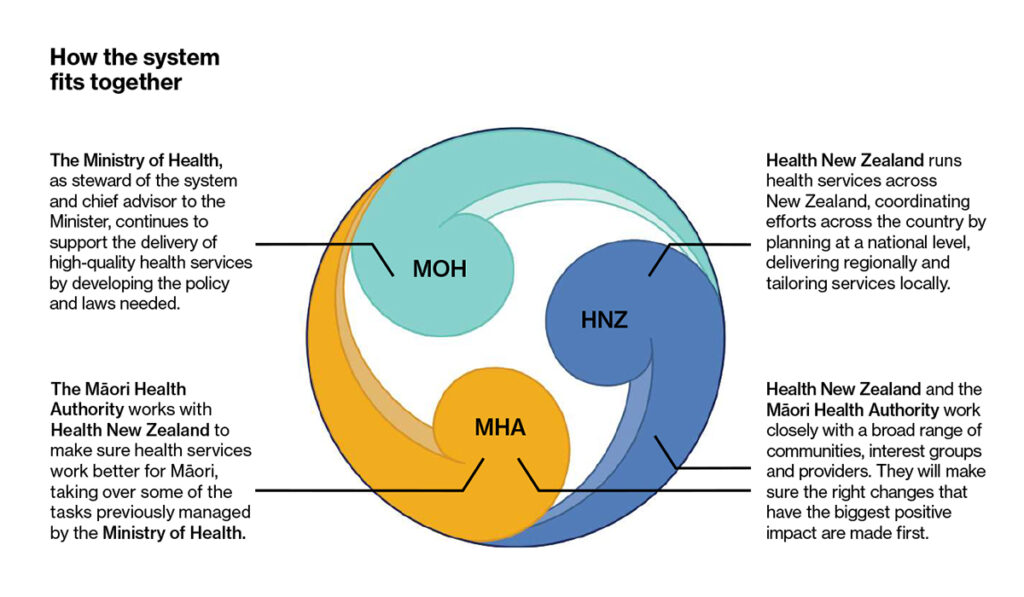
The reforms will see a refreshed Ministry of Health (MoH ) continue to be the chief steward of our health system focusing on strategy, policy, regulation and monitoring, while two new entities Health NZ (HNZ) and a Māori Heath Authority (MHA) will forge a radical new direction in the way we provide services.
In an early online presentation to stakeholders, Margie Apa, CEO of the interim HNZ described the two new entities as being like a double-hulled waka, Te Tatou waka hourua, both heading for the same destination/vision Te Pae Tawhiti.
Keriana Brooking, former CEO of Hawke’s Bay DHB, puts it simply: “We’ll all be in the same boat. Neither will be able to move without the other.”
Health New Zealand replaces district health boards (clearing their combined nearly $1.8 billion in debt) and leads the functional operation of our newly-nationalised health system.
The Māori Health Authority is an independent entity with clear accountabilities to both Māori and Ministers. It will work with Health New Zealand to commission and plan services, commission kaupapa Māori services and monitor the performance of the health system for Māori.
“There will be a Māori voice in all health decisions going forward,” says Brooking. “Just as there’ll be a clinical voice. A consumer voice. A business voice…”
The Māori voice in Hawke’s Bay will be mediated, as in other regions, by an Iwi-Māori Partnership Board, which BayBuzz understands is being established as we go to press with members having to apply and then be recruited to the Board. Its membership comprising iwi from around HB, including our largest, Ngāti Kahungunu, as well as post-Treaty Iwi Settlement groups and others.
I tried to contact chief executive for Te Taiwhenua o Heretaunga, Waylyn Tahuri-Whaipakanga who I understood had been participating on the design work for our Iwi Māori Partnership Board. She didn’t respond to my requests for an interview.
However, Phillipa Blakey, chief executive officer of the Primary Health Organisation, Health Hawke’s Bay, told me the Partnership Board would be across all health services in Hawke’s Bay and would connect into ‘Localities’.
Local priorities
Localities are a core part of the reforms. Eventually all New Zealanders will be assigned to geographical localities. In HB these will echo our current physical divisions: Wairoa northern HB; Ahuriri Napier, Heretaunga Hastings, Central Hawke’s Bay.
Within their Localities, the new Iwi-Māori Partnership Boards, service providers, health and wellbeing agencies will all work together to determine the priorities and the roll out of services for their community. For example, one Locality might have a need for more diabetes support – and it will be up to local partnerships to agree on whether dedicated services are commissioned. Another Locality may want to focus on more support for the elderly, and/or for its cancer patients.
Care and support in a Locality will be joined up across different health and wellbeing providers. For example, someone’s GP, local pharmacist and in-home nurse will work together to provide the wraparound care and support that person needs.
There are three strong features of the reform that come from a community perspective, says Brooking. “Establishing the Localities and how they work; the introduction of the Māori/Iwi Partnership Board and how they contribute around decision making to what is purchased, planned and delivered; and the role of the consumer.”
She says front-line staff [nurses, doctors, psychologists, carers] will get more involvement in decision-making within their Locality. “But they’ll have to share it with consumers, community groups and the Iwi-Māori Partnership Board.”
Localities are still being established and won’t be fully rolled out across New Zealand until mid-2024 but in April this year Wairoa was chosen as one of nine pilot Localities around the country to come up with a Locality Network Prototype. This offers some clues as to how Localities might function across Hawke’s Bay.
Wairoa has created a working group of iwi, government and service providers including members of Tātau Tātau o Te Wairoa (the Treaty Settlement Group), members of Whānau Ora, Wairoa Taiwhenua and the former DHB to deliberate on how the community of 9,000 pop wants to run its future health services.
Wairoa Council CEO and chairperson of the working group, Kitea Tipuna says access to health services has been an ongoing problem for the area and is now their prime focus. “We will be asking how do our communities access services and be self-determining? What does that look like? And what might this look like for our different groups such as kaumātua, tamariki; those with long term health conditions and our rural communities including Nūhaka, Māhia and Mōrere as well as for our online services.”
Some of the potential gains for all New Zealanders from the reforms should be apparent fairly quickly, says Brooking. She offers the example of someone awaiting a hospital procedure.
“If I was in Northern HB and couldn’t get my cancer treatment done in Wairoa, I would go to Palmerston North as has traditionally happened or, now there is no reason why I couldn’t go to Gisborne, where I might have good whānau support. Or if Gisborne people usually go to Waikato for hospital services, they might choose to come here to Hawke’s Bay instead. So, some of the boundaries constructed through the DHB legislation will get removed.”
MP Lorck says she has people coming to her office all the time complaining that they can’t get a hip or knee replacement. “These reforms are for those people too. In time, because we are no longer restricted by our boundaries and DHBs competing against DHBs, if you need a new hip in HB and there is someone in Palmerston North who can do it, you’ll be able to get it,” Lorck says. “Also, if you are from HB but have an accident in Auckland your records will be in the national database.”
It has even been suggested by NZ Health interim CEO Margie Apa that over time health professionals might be the ones moving around. “If we’re really doing well, we might have teams of people who might fly out, for example, to Tairāwhiti to clear a list of cataracts.”
Other than the above, some of the main changes promised by the reforms include:
• a greater range of care and support available for people in their local communities, with more care provided outside of hospitals;
• services such as general practice, well-child teams, pharmacists, dietitians, physiotherapists and hauora Māori providers working more closely together in their communities;
• more options for whānau to access kaupapa Māori and other appropriate services;
• better access to consistent and high-quality emergency and specialist healthcare, available to everyone, no matter where they live;
• more virtual and digital services available to support the system, such as phone and video consultation; and,
• more opportunity for NZers to get involved in designing health and wellbeing through participation in local planning and the opportunity to engage in national consumer forums.
Local reaction
But what do our Hawke’s Bay doctors and health providers think?
The reforms are aspirational, says Jon Eames, a former owner of Te Mata Peak Practice, now working part-time as a contract GP at Central Medical in Marewa. “But the devil will be in the detail,” he cautions.
Eames is keen to see how well primary health care will be supported and resourced by Health NZ Regional Boards – also part of the reformed infrastructure. He is glad we are getting rid of the postcode lottery system that led to different treatment priorities in different DHBs. “But if we give everybody equal access to hips and knee replacements, for example, then what’s going to miss out?”
For David Rodgers, a GP at Tamatea Medical Centre, and Hawke’s Bay representative on the New Zealand Royal College of General Practitioners, the reforms all seem very high-level at this point.
“On the ground we have a massive GP recruitment crisis. In HB we’re currently 28 GPs short and far too many people don’t have a GP and will struggle to access all sorts of healthcare.
“We’re a depleted workforce,” Rodgers continues. “We limped through Covid and now there is a big wave of pathology that we need to deal with. We need help right now. We need a magic GP tree.”
He jokes, but the sense of urgency in his voice is evident.
“It’s hard for people in high positions in the health system to understand what it takes to get GPs bedded into the community. It’s not like shifting a brain surgeon around from hospital to hospital; there’s a whole community the GP needs to relate to.”
Rodgers sees the Hawke’s Bay and wider New Zealand GP crisis as a failure of planning and funding. “Not enough GPs have been trained and there hasn’t been enough funding for core GP business. NZ-wide we are at about 74 GPs per 100,000 while Australia is at 100 GPs per 100,000 – and that is where we need to be.”
So Rodger’s greatest hope is that the new HNZ will make recruiting doctors at a national and international level a top priority. On balance he is in favour of the health reforms. “The new model will lead to far better community-led commissioning of health resources – and that is exciting.”

The intention is good and the focus on equity is absolutely right but we know the execution is the hard bit Is this just shifting chairs on the Titanic We dont know yet and its going to take a long long time to embed the changes
SHANE GORST GENERAL MANAGER TŌTARA HEALTH
Shane Gorst, general manager of Tōtara Health, which has primary healthcare clinics in Hastings and Flaxmere, says the ideology of the reforms is good.
“The intention is good,” he says, “and the focus on equity is absolutely right, but we know the execution is the hard bit. Is this just shifting chairs on the Titanic? We don’t know yet and it’s going to take a long, long time to embed the changes.”
He says it is discouraging to be on the front-line watching and at the same time having to do more with less. He points to the recent loss of the DHB contract for free GP visits for 14-17 year-olds. Tōtara Health has commited to self-fund the service anyway, in the same way it self-funds GP consults for women under 30.
If anything, Gorst’s prime concern is the current GP funding mechanism – ‘Capitation Payments’ – which allocates funding to GP practices based on a per person system. On average, when combined with the patient’s co-payment, that’s basic funding for about three and half doctor visits per person, per year. “The funding needs to be targeted where it is needed,” he says. “So for us how the reforms set up the new funding and support mechanism will be key.”
Tōtara Health was founded in Flaxmere almost 40 years ago and today it has 7,000 Māori patients and 2,000 Pacifica, and is the largest provider of primary health care to Māori and Pacifica in Hawke’s Bay.
“Our Māori and Pacifica whānau currently have choice and we hope it stays that way,” says Gorst. “Many of our whānau have been coming to us for generations.
“We are hopeful there will be improvements with the reforms and that the system will have at its core a ‘by Māori for Māori’ approach with organisations like ours wrapping around that, taking a ‘with Māori for Māori’ approach.
“We must find ways for Māori organisations and non-Māori organisations, private and public, to work together in authentic partnerships,” he adds. “And for them to be grounded in high trust relationships.”
Nathan Harrington says Te Kupenga Hauora hasn’t seen much detail on the reforms yet and is “adopting a wait and see approach”. But he hopes his organisation will be a voice within its ‘Locality’. He is aware there is some scepticism about the Māori Health Authority.
“But look at Māori Health providers and how we responded to Covid,” he says. “The way we’ve managed to engage with hard to reach-whānau by using whanaungatanga (relationships) and whakapapa (genealogy) in the community to get vaccination rates up.”
Covid has also forced providers to partner up with other providers “rather than being competitive and working in silos,” says Harrington. “For example, in Ahuriri, Te Kupenga Hauora and Māori providers, funders, Taiwhenua and iwi partnered up to get food out to whānau during the lockdown.
“I am hopeful and optimistic that this is the best way forward and that the most important voice in the new system will be whānau so that what is being delivered is meeting their needs.”
If anyone could steward Hawke’s Bay through the first bumpy phases of the health reforms it would surely be Keriana Brooking, our former DHB CEO. I sat down with her in mid-May as she told me she would be staying after 1 July and that all her staff would move over to employment with either HNZ or the new MHA. (View that interview online at: www.baybuzz.co.nz/dhbs-ceo-keriana-brooking-on-health-reforms/)
But two weeks on, as BayBuzz was tight on deadline, I received an email from the DHB Communications team: “Keriana Brooking has now been seconded into Interim Health New Zealand as National Director Commissioning – this is a temporary role expected to last two months.
“Andrew Boyd is now Acting Chief Executive for HB DHB until 30 June,” I was told, “and from 1 July will be known as the interim District Director. There will be no CEO roles in the districts or regions.”
Brooking was already in Wellington, I learnt, and Boyd is the former chief financial officer for Hawke’s Bay’s outgoing DHB.
So things are changing fast, and we can expect more changes as the reforms roll out. We’re told even Health New Zealand (HNZ) and the Māori Health Authority (MHA) are only “placeholder” names and by July l these will have changed too as a visual identity and logo is revealed for the new entities.
During my interview with Brooking in mid-May, I had asked her what Hawke’s Bay might look like 10 years down the track if the health reforms bedded in properly.
“In all corners of Hawke’s Bay consumers will understand all the services that are available to them and how to access those,” she said. “Like other industries we will have real interaction on how services can be different and better. Not just because someone has sent us a complaint but because a good service industry has a person-centered voice.
“We will see quite a dramatic shift in the use of digital technology in our health system. Ten years ago, we couldn’t have imagined we’d be giving out pulse-oximeters during Covid. So, ten years from now there will be things we haven’t even thought about.
“The way our hospital looks and feels will be more conducive to people who need to use those services. In HB we will still have a marae and chapel, but we will be all over sustainability, using our footprint wisely.
“We are concerned about the lack of GPs and work is going on to fix that. We would like nurses pay equity to be settled, immigration to allow more nurses in and initiatives for more nurses to go through training and graduate.
“Above all,” Brooking stresses, “we will have a more streamlined health system.”
Watch this space.



I am a retired medical practitioner with 36 years experience as an anaesthetist in Hawkes Bay.
When I qualified I swore the Hippocratic Oath to treat all people in need regardless of race, colour or creed.
Nothing has changed . We should be treating the people in need.
Modern technology enables us to identify those most at risk, we know the interventions that are required, we can move the resources to perform those interventions
Setting up 2 very expensive bureaucratic machines which will be competing for resources is purely ideological and will do nothing to help the people at the coal face who actually do the work
This whole restructuring should be canned and the people who actually do the work consulted, not the idealogues
Matt Cambell has completely summed it up why does this govt continue to copy the mistakes made elsewhere? Race based anything is destructive and I can’t believe its happening here in NZ and we can’t stop it because we no longer have a democratic voice. Time to leave – how very sad.